
Edifecs, A Cotiviti Business, provides market-leading technology to enable its payer and health system customers to unlock greater value with their healthcare operations solutions and data management platform, which includes its award-winning healthcare interoperability cloud solution. Edifecs healthcare SaaS solutions serve as the foundation that eliminates stakeholder friction to overcome healthcare’s biggest challenges, including accelerating value-based care adoption and obtaining more complete and accurate care funding. For more information, visit www.edifecs.com.
Healthcare Data Interoperability
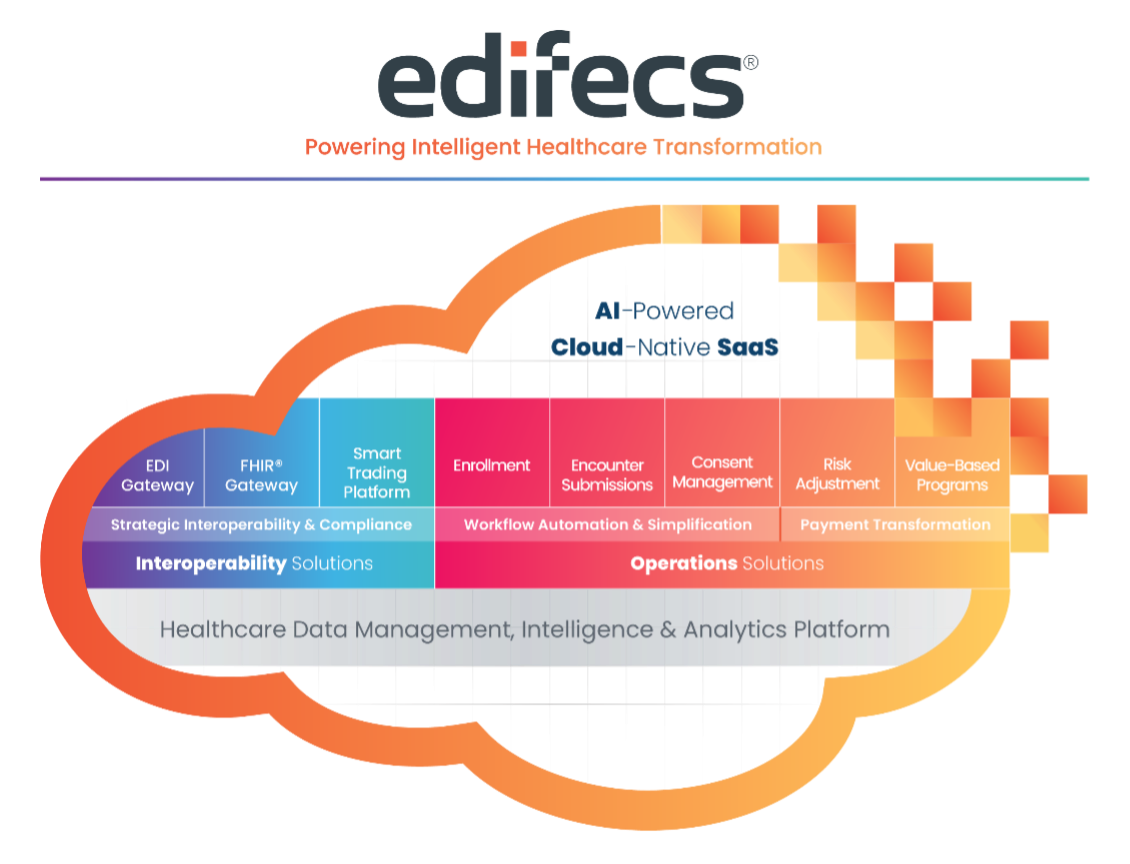
The Edifecs Healthcare Interoperability Cloud combines our EDI, FHIR, and Smart Trading platforms to seamlessly connect systems, processes, organizations, and people across the entire healthcare ecosystem.
· EDI Gateway
Optimize data processing, reduce interoperability workloads, and support all X12 HIPAA-compliant transactions with a single EDI solution.
· FHIR Gateway
Comply with CMS Interoperability mandates 9115 and 0057. Reduce provider abrasion and improve ALR by orchestrating FHIR-based electronic prior authorization submissions.
· Smart Trading Platform
Automate business processes, modernize your technical infrastructure, and reduce costs.
Workflow & Data Enrichment
The Edifecs Healthcare Operations Cloud enables users to holistically apply their data across the major facets of their business to support the entire member journey—from contracting and enrollment through encounter submissions and prior authorizations.
· Member Enrollment
Simplify and streamline enrollment management processes to capture a greater market share across all lines of business.
· Encounter Submissions
Break down encounter operations silos, support submission accuracy, and ensure compliance
· Member Consent Management
Effectively manage member consent by capturing and enforcing federal, state, CMS, and enterprise data-sharing policies according to member preferences.
· Risk Adjustment
Maximize your resources to find more risk-adjustable opportunities faster and ensure ongoing compliance.
· Value-Based Payments
Design, automate, and administer value-based contracts for more accurate payments and faster scaling of value-based programs.
